Cardiovascular and Angioplasty Drapes
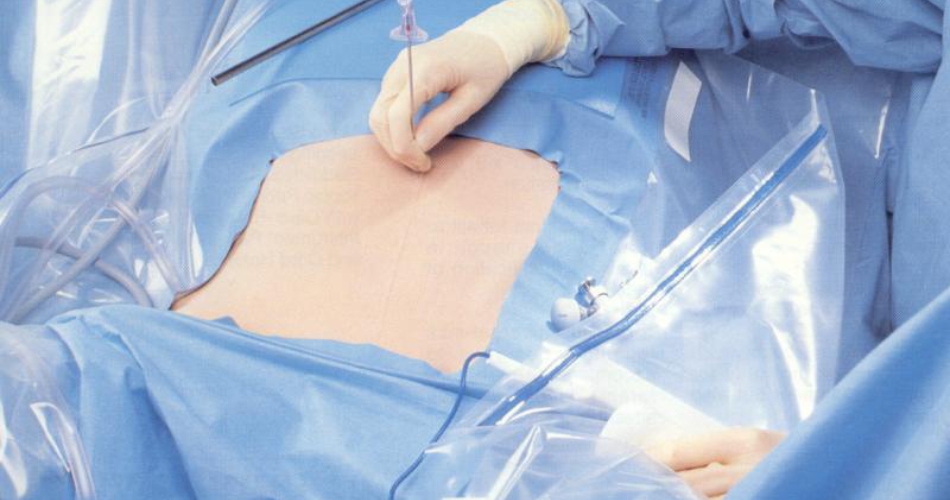
Cardiovascular surgery is used to treat complications of ischemic heart disease (for example, with coronary artery bypass grafting); to correct congenital heart disease; or to treat valvular heart disease from various causes including endocarditis, rheumatic heart disease, and atherosclerosis. It also includes heart transplantation.
While Angioplasty is a minimally invasive, endovascular procedure to widen narrowed or obstructed arteries or veins, typically to treat arterial atherosclerosis.
Both cardiovascular and angioplasty surgery are delicate surgical procedures that can not be conducted without the use of drapes. While the surgeons and the operation team use scrubs which are lint-free and comfortable to wear, as an effective barrier against pathogens to reduce the risk of infection.
Drapes are used to prevent microorganisms from invading the sterile field by covering the area surrounding the probable surgical wound thus avoiding further complications.
After antiseptic skin preparation, surgical drapes are placed over the surgical site to maintain a sterile field and to prevent contact with untreated surfaces. One of their most important features is fluid containment. Other requirements for sterile surgical drapes include resistance to microbial penetration (dry, wet), their absorption capacity, their resistance to liquid penetration and tensile strength.
As microorganisms on patients' skin are a major source of contamination, using draping materials plays a pivotal role in reducing infections and improving patient outcomes. Surgical drapes create an effective physical barrier for preventing the microbial transfer from both the patient and the environment to the wound.
Surgical drapes (made from nonporous material) designed for cardiovascular and angioplasty surgeries provide efficient infection control featuring effective fluid control to maintain a dry working area. This is because during surgery, body fluids and irrigating solutions come into contact with the drapes, and the risk for pathogen transmission increases when the materials become moist or wet.
Since these surgeries are usually long the drapes used should be light, soft to touch, allow the much-needed air circulation to maintain optimal body temperature. Draping material must also be low-lint, as lint can transport microbes and introduce them into the surgical wounds, increasing the risk of infection.
Surgical drapes that resist liquid penetration and remain effective barriers when wet should be used to avoid infection acquired from blood-borne pathogens. Disposable drapes, gowns, gloves and sponges that are contaminated with blood should be discarded in special containers and labeled as healthcare waste.
The drape should be preferably made from a generally rectangular main sheet of a flexible, fluid repellent nonwoven fabric and the fenestration area should be largely centrally located in the length and stretches from near the end of the patient's foot to the head end of the patient at least past the chest area. An additional reinforced work area should be provided at the patient head directed end.
As an alternative to reusable scrubs, that need to be washed frequently to remove contamination, disposable scrubs provide numerous advantages. Freshly unpacked, the risk of contamination by clothing particles is significantly lower, it provides an effective barrier against germs.
Related Blogs
 Surgical Drapes and Gowns: A Surgical Revolution
Surgical Drapes and Gowns: A Surgical Revolution
 Battling Infection and Germs: Disposable Gowns vs Resusable Gowns
Battling Infection and Germs: Disposable Gowns vs Resusable Gowns
 Risk analysis of Disposable Surgical Drapes
Risk analysis of Disposable Surgical Drapes
 Surgical Disposable Drapes
Surgical Disposable Drapes
 Surgical gowns and drapes in the Operation Theater
Surgical gowns and drapes in the Operation Theater
 Surgical drapes and gowns for Orthopaedics and Traumatology
Surgical drapes and gowns for Orthopaedics and Traumatology
 Introduction to Neurology surgical drapes and kits
Introduction to Neurology surgical drapes and kits
 Drapes and Kits for Gynaecology
Drapes and Kits for Gynaecology
 Use of Drapes in Urology Treatment
Use of Drapes in Urology Treatment